
Sizable regulations enforced upon physician groups are holding practice executives to a glowing screen late nights and through the weekend. Practices are dedicating substantial hours and personnel to determine which value-based initiatives to focus on in the coming years in order to remain profitable.
One thing that remains true is that physicians who bill Medicare more than $30,000 in Part B and provide care for more than 100 Medicare patients a year are subject to the Quality Payment Program (QPP) of MIPS or APMs under CMS’s MACRA reimbursement regulations. Several details including practice structure, size, and reporting capabilities, will determine the category under MACRA in which it applies.
CONTINUE READING
Topics:
Closed-Loop Referrals,
MACRA,
Referral Automation,
Automated Referral Management,
MIPS,
CMS

Inefficiencies in the patient referral process plague practices by increasing the administrative burden on providers and front-office staff. Internests and family practicioners dedicate nearly 20% of their time to administrative tasks1 while practice managers and medical receptionists can waste up to 30 minutes on the phone chasing down patient information2. According to a paper in the International Journal of Health Services, "more extensive use of electronic medical records [is] associated with a greater administrative burden."
Disconnected practices are struggling to exchange clinical information and communicate securely without interruptive phone calls and faxes. Referral partners on different EHRs are left with lackluster options, such as sending transitions of care and last office notes into a Direct Secure Messaging void with hopes of receiving a consult report back.
CONTINUE READING
Topics:
Closed-Loop Referral Management,
Referral Workflow,
Referral Automation

Patient Centered Medical Home (PCMH) embodies the current trajectory of healthcare in that the patient is the focus of the medical model. The National Committee for Quality Assurance’s (NCQA) PCMH program is vastly adopted, with more than 12,000 practices, 60,000 clinicians, and 100 payors participating. In fact, 1 in 6 eligible physicians in the U.S. practices in an NCQA-Recognized PCMH.
With the objective to strengthen patient-provider relationships, reduce healthcare costs, and improve quality, NCQA continues to accelerate the growth of value-based care with the remodel of their PCMH program. Changes to the new PCMH model reduces the burden of the reporting process and focuses on increased healthcare quality and practice performance.
CONTINUE READING
Topics:
Care Coordination,
Healthcare Analytics,
Value-Based Care,
PCMH

Independent primary and speciality care practices have challenging years ahead. MACRA, MIPS, APMs, and the ACA are posing uncertain regulations and complicated payment models.
Despite this uncertainty, there is one thing that’s clear: independent practices must prepare to take on risk in order to stay profitable.
We sat down with Mark Kissinger, executive director of Genesis Medical Associates, to get the inside scoop on the challenges a large independent primary care practice faces in a value-based care and regulatory-driven world.
CONTINUE READING
Topics:
Care Coordination,
Coordinated Care,
Referral Network,
Closed-Loop Referral Management,
Value-Based Care

Once considered a critical component of meaningful use, DSM (Direct secure messaging) within an EHR poses significant limitations to referral management. While it conveys information electronically within a practice, DSM alone does not provide for comprehensive data exchanges between PCPs and consulting physicians. The Journal of General Internal Medicine notes that communication breakdowns affect care delivery between two practices on different systems. Specialists report that, 86% of the time, they do not receive information from the PCP prior to the referral visit. Additionally, poor referral tracking leads to inappropriate or unnecessary referrals and inefficiencies in care delivery. DSM in EHRs presents inevitable challenges for both primary and specialty care practices.
CONTINUE READING
Topics:
Care Coordination,
Referral Management,
DSM,
EHR

Communication between primary care physicians (PCPs) and the specialists they refer patients to is paramount to the overall best outcome for the patient. Much of the communication breakdown lies in outdated protocols and manual workflows that some organizations continue to employ. In the past, many physicians referred patients to various specialists, but never followed up on the recommendation. The patient was left to make their appointment with the specialist. In those cases, as high as 50% of the patients never made the appointments or followed up on the physician's recommendation. As illustrated, improving referral adherence shouldn't solely be the responsibility of the patient.
CONTINUE READING
Topics:
Coordinated Care,
Referral Adherence,
Care Transitions

Former President Barack Obama and former Vice President Joe Biden both care a great deal about digital health technology systems. Even when they had less than two weeks left in the White House, physicians' ability to share patient health records digitally was top of mind — and on the same day, too!
According to Politico’s Morning eHealth newsletter, it was “the first time since the gods called this newsletter into existence [that] President Barack Obama and Vice President Joe Biden both talked on the same day about health IT”.
CONTINUE READING
Topics:
Coordinated Care,
Referral Network,
Interoperability,
HIT,
Healthcare Data,
Care Transitions

The traditional patient referral process is broken. Its primary shortcomings - poor communication and follow-up - have far-reaching consequences.
Consider these stats: Only half of referrals result in a completed appointment, according to the Archives of Internal Medicine. The Journal of General Internal Medicine found that, while 70% of PCPs report sending information to specialists, only 32% of specialists receive clinical information before seeing the patient. An Archives of Internal Medicine study shows that PCPs report not receiving consult reports about 40% of the time; and when reports are sent, the Journal of General Internal Medicine adds, they arrive at least seven days after the patient visit in 64% of cases.
CONTINUE READING
Topics:
Referral Network,
Referral Management,
Patient Adherence

The loop in communication and clinical documentation between healthcare providers has traditionally been open for many organizations. Often when referrals are made, they are left largely to the patient to schedule. Many physicians may not even check whether the patient was seen by the specialist until the patient's next appointment or if contacted for records.
There are a million moving parts to the healthcare landscape today, so it's understandable that follow up with referrals might slip through the cracks without a proper protocol. Unfortunately, the cost of poor care coordination can be exorbitant - for the patient's own health and for the physicians and organizations involved.
CONTINUE READING
Topics:
Care Coordination,
Referral Management,
Provider Accountability,
Direct secure messaging

What you don’t know can hurt you.
When practices fail to manage a standard and consistent patient referral process across all locations, patients get sicker. And when PCPs and specialists aren’t on the same page about a patient referral, urgent health conditions worsen while important diagnoses get missed or delayed.
But a defective referral communication process isn’t just a big problem for patient care - it’s also a big problem for medical practices’ morale and bottom lines. Practices often get sued for medical negligence when a patient referral falls through the cracks.
Referrals play a role in an immense number of medical malpractice claims. Patient handoffs in medical settings contribute to 20% of diagnostic errors that lead to malpractice suits1.
CONTINUE READING
Topics:
Referral Management,
Closed-Loop Referrals,
Malpractice

A critical, but often-overlooked, aspect of the referral process is cultivating provider partnerships that facilitate referrals and enhance the continuum of care. The continued emphasis on value-based care will result in increasing numbers of physicians working together to coordinate care, especially for patients with chronic conditions. While the traditional referral system is generally regarded as inadequate, best practices can help you optimize working relationships with collaborating physicians.
CONTINUE READING
Topics:
Referral Network,
Referral Management

Effective communication is at the heart of success or failure in patient care. This is never more evident than in the relationship between Primary Care Physicians (PCPs) and the Specialists they refer their patients to for follow up examination. The best PCPs provide their patients with an ongoing relationship - they serve as a mentor or partner in health, helping patients understand their specific needs and making recommendations when appropriate. The benefit for patients in developing long-term relationships with their PCP is that they have a trusted physician who knows their history and can more easily assess warning symptoms for new ailments and lifestyle changes appropriate for health risks.
CONTINUE READING
Topics:
Coordinated Care,
Care Transitions

Over the past decade, as healthcare organizations began to implement electronic referral management applications, studies were conducted to measure their overall functionality and value in patient care and satisfaction. The results proved that when handled properly, electronic referral management cured several problems inherent in the old paper-based coordination of care procedures. What emerged from years of trial and error was a clear set of best practices for both primary and specialty care facilities that keeps the patient front and center.
When a healthcare organization decides to implement an ERM, what are those best practices to keep in mind?
CONTINUE READING
Topics:
Referral Management,
Referral Workflow
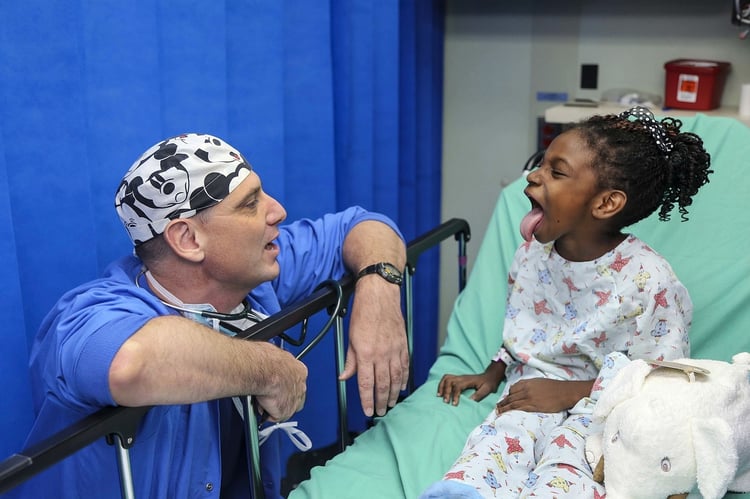
Today's healthcare model requires that services be patient-centered. Additional challenges arise, though, when care needs to be coordinated among multiple providers. From 1999-2009, the number of primary care visits resulting in a referral increased by 159%. Research strongly indicates that referring physicians need to improve the quality of information they provide to consulting physicians. When surveyed, 63% of PCPs and 35% of specialists report dissatisfaction with the current referral process. Paper referrals often do not provide adequate information. In other cases, consult reports are not delivered in a timely manner. Many referrals do not even include transmission of information, either to or from specialists.
CONTINUE READING
Topics:
Patient Satisfaction,
Referral Workflow

Relationships between PCPs and specialists are sacred. On average, a single PCP is connected to 68 specialists. However, lack of electronic connectivity makes it difficult to coordinate care and manage referrals—apart from hiring additional administrative staff.
Without patient referrals from PCP to specialist, it is estimated that only half as many patients would show up to their specialty care appointment1. Furthermore, “self-referral” patients who see specialists without recommendation from a PCP are associated with higher patient dissatisfaction and poorer continuity of care with the primary care doctor2. As PCPs refer more patients to specialists each year, coordinated care and automated referral workflow become an urgent issue for both independent and hospital-based practices.
CONTINUE READING
Topics:
Care Coordination,
Referral Network,
Referral Adherence,
Referral Workflow

With coordination of care a major aspect of healthcare delivery, mistakes in the process lead to patient dissatisfaction or possibly worse. An excess of frustration in a patient's experience often leads them to pursue other primary care options. Fortunately, the emergence of electronic referral management technology can reduce errors significantly when referring to network specialists. The advantages of an electronic referral network can be seen and measured within those HCOs that adopted them early. As medical enterprises continue to implement the systems, better care coordination and happier patients will be the result.
CONTINUE READING
Topics:
Coordinated Care,
Referral Network,
EHR

As value-based care takes center stage in healthcare, primary care providers (PCPs) and specialists must find ways to eliminate communication deficiencies and share information more effectively to ensure a more well-rounded and positive patient experience. Strong quality scores, efficient operations, and credible customer service are no longer just admirable traits of a positive care coordination environment; they’re quickly becoming characteristics that define whether primary care succeeds or falls short in value-based care.
CONTINUE READING
Topics:
Care Coordination,
Referral Management,
Referral Workflow

Care coordination missteps are damaging to providers across the healthcare industry and one huge, overarching mistake is apparent: not enough information is being shared. A study by Health Affairs shows that only 14% of physicians share information with providers outside of their organization.
Unfortunately, care coordination mistakes can be costly...and not just in terms of financial expenses. Some of the most common care coordination mistakes are also major culprits for death and exacerbated patient health problems. U.S. News & World Report indicates, “Medical errors are [the] third leading cause of death in the U.S. 10 percent of U.S. deaths are due to preventable medical mistakes.”
We’ve identified six areas of care coordination where many practices make mistakes -- check out what they are, and see how many apply to you.
CONTINUE READING
Topics:
Care Coordination,
Care Transitions,
Referral Workflow

An alarming number of primary care practices don’t have the staff required to proactively manage referrals. Medical assistant teams lack the capacity required to manage chronic care and quality programs, meet payor requirements, and hunt consult reports from specialists. As a result, these practices manually track referrals only when they are required to for regulatory requirements or internal referral initiatives.
The primary care practices that are proactively managing referrals are doing so with an overwhelming amount of expensive and manual workflow. Care coordinators are adding hundreds of hours to their workflow each month to ensure that patients are completing their appointment and that specialists are returning the clinical information needed for appropriate follow up.
In contrast, primary care practices that automate their referral workflow electronically are recovering up to 70% of their staff’s time [1] spent manually managing referrals.
Improved referral processes help practices meet value-based initiatives and devote time to programs that drive revenue—like preventative and chronic care management.
CONTINUE READING
Topics:
Coordinated Care

Healthcare reform is very real. Only primary care practices who prepare now will be ready for big changes in reimbursement and quality metrics. According to Dr. Danyal Ibrahim, the Chief Data Analytics officer at Saint Francis Care in Connecticut, identifying gaps and bringing data together is crucial to overcoming isolated silos in healthcare and to delivering the kind of outcomes that meet and exceed performance metrics.
Providers who don’t harness data for the new era of healthcare “have at least a vague, nagging feeling that they should probably start developing the data-driven competencies.” In a recent HealthITAnalytics article, Dr. Ibrahim described identifying and overcoming data silos as the biggest hurdle of creating a streamlined data analytics infrastructure. “[T]here are so many times when our data ends up siloed, and pieces of information end up going to all different places that cannot communicate with one another...So one big component goes to the finance department, and other to IT, and another to the quality improvement team.”
Forbes magazine weighs in on poor data sharing as “a medical tragedy of underappreciated dimension. Valuable, even vital information often remains uncaptured, unanalyzed, and, especially, unshared.”
Overcoming health data silos is proven to lead to cost savings. A McKinsey Global report estimated that the efficient use of data in healthcare could create more than $300 billion in value every year and quintuple hospital profits.
CONTINUE READING
Topics:
Referral Management,
Healthcare Data,
Referral Management Analytics

Value-based care models are said to represent “policymaking at 80,000 feet.”
Healthcare leaders who were once optimistic about value-based reimbursement models are becoming doubtful after seeing the performance of several programs. Accountable Care Organizations (ACOs) are achieving modest gains and a meager 28% of Medicare Shared Savings Program (MSSP) participants have generated cost savings.
CONTINUE READING
Topics:
Care Coordination,
Referral Management,
Population Health

Image courtesy of flickr
Problems with handoffs are a big deal in clinical practice. Defective handoffs lead to patient harm, treatment delays, inappropriate treatment, and longer stays in the hospital. In a typical patient handoff between physicians, important patient information is often not given to physicians who take over care of a patient. In a hospital, “[s]hift changes, also known as handoffs, are prime opportunities for key information about a patient’s condition to get lost in the shuffle,” according to a recently released study about patient handoffs in JAMA Internal Medicine [1].
CONTINUE READING
Topics:
Care Coordination,
Healthcare Analytics,
Referral Management,
Healthcare Data,
Care Transitions

Electronic health record (EHR) rollouts are huge undertakings. It cost Massachusetts General Hospital $1.2 billion to shift towards Epic Systems’ EHR over the last three years. And the rollout has been complicated. They had to keep their old, homegrown systems running at the same time while they switched to their new EHR system. On top of that, they had to conduct extensive data conversions, testing and staff training.
Outpatient physician practices don’t fare much better with EHR rollouts. Outpatient EHR system implementations are estimated to cost $46,569 per physician. And one study of 49 PCP practices determined that the average 5-year return-on-investment of an EHR system was a loss of $43,743 per physician. 73% of the surveyed primary care practices demonstrated a negative ROI from EHR systems over 5 years.
CONTINUE READING
Topics:
Referral Management,
EHR

Hospitals and Health Networks Magazine recently championed the concept of primary care physicians and specialists working closely together as partners, rather than continuing disconnected referral relationships.
Partnering with Primary Care
H&HN’s article touts the increased efficiency and improved patient care in organizations with tightly aligned specialty and primary care partners.
CONTINUE READING
Topics:
Referral Management,
Interoperability,
HIT,
Referral Management Application

Healthcare practitioners want to provide the best care for their patients both during and after office visits. But one major stumbling block is that the majority of physicians in the United States aren’t capable of sharing information electronically outside of their practices. Data shows that the majority of primary care practices are struggling to seamlessly share patient information, efficiently manage referrals, and facilitate interoperable communication with specialist partners.
CONTINUE READING
Topics:
Referral Management,
Interoperability

A recent article in technology and business magazine Fast Company heaped praise on user-friendly applications that go beyond electronic health record (EHR) systems. The beginning of the article detailed a number of the pitfalls of EHR systems:
1. EHRs were not set up for patient care
One pitfall of EHRs outlined in the Fast Company article is that they “weren't designed to help their providers treat patients.” The article states that EHRs are more geared towards meeting regulatory requirements, maximizing billing and avoiding liability. The Meaningful Use program was implemented by the government in 2011 to incentivize adoption of EHR systems, but Meaningful Use has been criticized for rewarding usage of EHRs rather than rewarding better patient outcomes.
CONTINUE READING
Topics:
Referral Management,
Referral Management Application

Healthcare reimbursement is undergoing “the most dramatic shift in Medicare payments in the program’s 50-year history,” from fee-for-service to value-based care. But most physicians aren’t familiar with the important law that is establishing these changes for the future, the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA). Proposed details for MACRA were released by the Centers for Medicare and Medicaid Service (CMS) a few months ago, in April 2016.
CONTINUE READING
Topics:
Referral Management,
Value-Based Care,
MACRA

Journalist Fareed Zakaria is certain that those who prevail in tomorrow’s health care arena are the ones who figure out how to use the troves of data at their fingertips to distinguish themselves from competitors.
“[W]hat you do with that data will probably be the key differentiator going forward,” Zakaria explains at a recent healthcare conference, the Health Forum and American Hospital Association Leadership Summit.
CONTINUE READING
Topics:
Healthcare Analytics,
Referral Management,
HIT,
Healthcare Data

Courtesy of Youtube
You may have seen the news that well-known infomercial psychic Miss Cleo, whose actual name was Youree Harris, recently passed away from colon cancer at the age of 53. She died while she was surrounded by her friends and family after entering into hospice care.
Here’s an old commercial of hers:
CONTINUE READING
Topics:
Patient Adherence,
Colorectal Screening

Entirely paper-based healthcare is going the way of the dodo bird. Since 2008, the number of office-based physicians who have adopted electronic healthcare records (EHRs) has doubled from 40% to over 80%. In fact, the number of physicians using EHRs has actually quadrupled in the past 12 years.
Poorly handwritten prescriptions are no longer a problem for the 70% of physicians who now prescribe medications for their patients electronically. The advancement of e-prescribing has led to a reduction in medical errors and prevents fraud, such as opioid abuse.
In addition, telehealth is booming, robotic surgery is more common, and robots are even roaming the hallways of hospitals to deliver food and transport trash.
CONTINUE READING
Topics:
Referral Network,
Closed-Loop Referral Management,
Closed-Loop Referrals,
HIT

DSM is antiquated, backwards, and “meaningless work for meaningful use” - Physician testimony | ONC HIT Policy Committee
“ONC’s new ‘interoperability roadmap’ downplays the potential of Direct messaging” as a solution for interoperability - Medical Economics
Contrary to what some electronic health record (EHR) proponents believe, DSM (Direct secure messaging) by itself is an unpopular and ineffective solution when it comes to true interoperability, care coordination and referral management. It has almost no practical benefit for referral management beyond what primary care practices use it for right now: getting credit for Meaningful Use stage 2.
CONTINUE READING
Topics:
Referral Network,
Referral Management,
Direct secure messaging,
DSM

As the CDC sounds the alarm to increase awareness for colorectal cancer screening, primary care practices find that their EHRs can’t support the task of getting patients to complete colonoscopy referrals. In addition to the CDC, there is a growing focus by medical societies, advocacy organizations and media personalities like Katie Couric to ensure that adults over 50 get referred for colonoscopies to detect and prevent colorectal cancer. Awareness initiatives are critical because half of all patients referred for colonoscopies fail to complete the procedure.1
CONTINUE READING
Topics:
Coordinated Care,
Referral Management,
Closed-Loop Referrals,
Referral Adherence

The leading cause of blindness worldwide is diabetes. However, referral management makes a significant impact on saving the eyesight of diabetic patients. Most people who have diabetes for more than 20 years develop diabetic retinopathy1, a condition where elevated blood sugar damages the blood vessels inside the retina. Over 7.7 million American adults have diabetic retinopathy today and that number is expected to double by 2050. The condition affects almost 30% of the US diabetic population over the age of 402 and causes up to 24,000 new cases of blindness in the US each year.
CONTINUE READING
Topics:
Coordinated Care,
Healthcare Analytics,
Referral Management,
Closed-Loop Referral Management,
Patient Adherence,
Diabetic Eye Exam
8 out of 100 missed or delayed cancer diagnoses are a result of a failure of a requested referral to occur.1 Furthermore, a recent study found that the risk for colorectal cancer almost doubles when a patient with a positive stool test waits over a year to have a colonoscopy.2 Colorectal cancer is the second leading cause of cancer-related deaths in the United States3 and up to 90% of colorectal cancer deaths are preventable with early detection.4
A significant amount of gastroenterologist referrals are for colonoscopies.5 But for every two patients who are referred by their physician to get colonoscopies, only one of them will end up getting the colonoscopy.6
CONTINUE READING
Topics:
Care Coordination,
Referral Management,
Closed-Loop Referrals,
Patient Adherence

Updated February 2017
In almost every speech given in 2016, Andy Slavitt, the former Acting Administrator for the Centers for Medicare and Medicaid Services (CMS), has emphasised the priority of closing referral loops to strengthen patient care coordination.
Independent practices have less than a year to prepare for newly developed value-based care reimbursement guidelines. The option to test the quality payment program under MIPS and MACRA will no longer be in play beginning in 2018. In view of the challenging financial penalties of value-based payment, many practice leaders are struggling to find an efficient way to close referral loops.
CONTINUE READING
Topics:
Referral Management,
Closed-Loop Referral Management,
Interoperability,
Closed-Loop Referrals

It would be easier to coordinate team-based medical care on facebook rather than with EHR systems.
- John Halamka, CIO | Beth Israel Deaconess Medical Center and co-chair of the federal HIT Standards Committee, at the HIMSS conference in March 20161
EHRs aren’t enough
A common misconception is that an electronic health record (EHR) can close referral loops and provide high-performance referral management for primary care practices. However, not long after EHRs were implemented, users quickly realized that EHRs alone are not able to establish a pipeline that allows data to flow between PCPs and specialists from different organizations.2
CONTINUE READING
Topics:
Care Coordination,
Healthcare Analytics,
Referral Management,
Closed-Loop Referral Management,
Interoperability

Accountability in health care often means that primary care practices are liable for the cost and quality of a patient’s care across the continuum of care. In the old, diminishing fee-for-service reimbursement system, practices were only reimbursed based on actions within their own office.
Now, in new reimbursement models like ACOs, PCMHs, risk-based contracting, and alternative payment models, shared accountability is king.
“The idea that you are accountable for what happens after people leave your office is no longer just a philosophical discussion. It's dollars and cents.”1
CONTINUE READING
Topics:
Referral Management,
Closed-Loop Referral Management,
Provider Accountability,
Value-Based Care

The New England Journal of Medicine describes the traditional patient referral process as a perilous journey [1]. Right off the bat, only half of patients show up to their referred specialty physician appointments [2].
In fact, the referral process is so fragmented that even when patients do show up to their specialist appointments, only 32% of specialists will receive clinical information from the PCP prior to seeing the referred patient. [3]
CONTINUE READING
Topics:
Coordinated Care,
Healthcare Analytics,
Referral Management,
Interoperability,
Closed-Loop Referrals

A tsunami of change is shifting the healthcare reimbursement system towards value-based care.
As a result of legislation passed in 2015, called MACRA, Medicare is supercharging its emphasis on value-based payments and the first performance year will be 2017. As a result, the way medical practices manage referrals will impact their revenue.
“Providers that hope to succeed under the new payment methodology need to begin making changes now.“
- Dave Wofford | Healthcare Financial Management Association
CONTINUE READING
Topics:
Coordinated Care,
Referral Network,
Referral Management

Care coordination is complex. Interoperability is far from reach. Patient information is difficult to track, especially when primary care physicians and specialists utilize different EHR systems. You need to stay competitive and make faster, smarter decisions. You want to fix these challenges, but you can’t because you don’t have the resources.
EHRs and practice management systems have referral order capability but are transactional and not built for true closed loop referral management. There is a difference between tracking and managing your patient referrals. So how are you going to manage health populations and improve patient care?
CONTINUE READING
Topics:
Coordinated Care,
Healthcare Analytics,
Referral Network








































