Entirely paper-based healthcare is going the way of the dodo bird. Since 2008, the number of office-based physicians who have adopted electronic healthcare records (EHRs) has doubled from 40% to over 80%. In fact, the number of physicians using EHRs has actually quadrupled in the past 12 years.
Poorly handwritten prescriptions are no longer a problem for the 70% of physicians who now prescribe medications for their patients electronically. The advancement of e-prescribing has led to a reduction in medical errors and prevents fraud, such as opioid abuse.
In addition, telehealth is booming, robotic surgery is more common, and robots are even roaming the hallways of hospitals to deliver food and transport trash.
Almost anywhere you look, the healthcare industry is making monumental shifts towards electronic processes. Despite the movement toward electronic systems, referral management has fallen far behind because EHRs don’t provide a robust referral solution, even if the EHRs have Direct secure messaging. Most primary care physicians still rely on inefficient paper referrals handed to their patient during an appointment. Patients are then expected to navigate the confusing and cumbersome healthcare system on their own.
Under current manual referral methods, only 50% of patients actually make it to their specialist appointments [1]. Manual and inefficient referral processes need to improve through online, standardized workflows. Referrals should be electronic too!
Shift from paper to digital healthcare
If you are part of a large physician practice, it’s likely you’ve adopted EHRs and use digitized healthcare practices such as e-prescribing. Beginning in 2011, the government funded up to $63,750 per physician to incentivize adoption and use of EHR systems through the Meaningful Use program. Since then, it has given out $34.7 billion through Medicare and Medicaid for electronic records adoption. That’s $2 billion more per year than the NIH’s funding for cancer research. Practices also face reimbursement penalties from Medicare for not having EHRs. And most recently in March 2016 New York State began to penalize all physicians who don’t send prescriptions electronically.
Inefficient medicine: too much paper and too many phone calls
See our roundup of recent studies that all touch on the manual methods that physicians still rely on today.
STICKY NOTES
One recent paper published in Applied Clinical Informatics found that 70% of doctors who use workarounds to follow-up on test results use paper, faxing or even sticky notes! Practitioners use paper as reminders by manually writing down test results that appear in their EHRs. They also write down information on paper because it is difficult to bring up the information in the EHR system after reviewing it the first time [2].
PAPER IS POPULAR
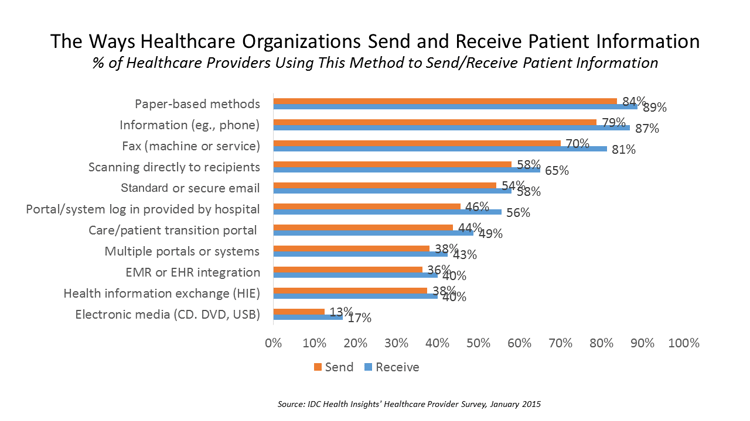
Market research from IDC released a survey that found that the majority of doctors still use paper transactions, unreliable faxes and manual phone calls to send and receive patient information. Paper was the most common method used, then phone, then faxes, and then scanning directly to recipients.
$8 BILLION IN UNNECCESSARY COSTS
CAQH, a non profit healthcare alliance, released its 2015 annual Index report that explored manual vs electronic transactions in healthcare. The report found “significant, unnecessary costs resulting from large volumes of manual transactions that could be handled electronically." It determined that manual transactions like phone calls and sending paper through the mail cost providers and plans $2 more per transaction than automated electronic transactions. Manual business transactions in healthcare cost $8 billion each year.
OMISSIONS AND ERRORS
One recent study in the Journal of the American Medical Informatics Association [3] found that EHRs reduced omission rates to 17.6% compared to 41.2% omission rates with paper medical records. Omissions occur when important information is left out of a patient’s record. For example, a patient with an irregular heartbeat might have no mention of it in a cardiac report.
Electronic referrals to the rescue
Moving to electronic health records from a paper-based health system is a complex process, but moving to an electronic referral system from a manual referral system is simple. For referral management, it’s easy and fast for practices to eliminate their paper-based referral ways and connect electronically with their specialist referral partners.
Most referral processes today rely on paper-based systems that consume too much time and effort, which causes unacceptable wait times [4] and inefficient specialty visits [5].
Joel Vengco, Executive Director of Clinical Information Systems at the Boston Medical Center, has called traditional paper and phone call-based referral management methods a fallible, cumbersome and broken-down process. The New England Journal of Medicine described the typical patient referral process as a “perilous journey through the health care system” [6].
Even when EHR systems have Direct secure messaging (DSM) functionality, the referral process is still perilous because DSM is a lousy solution for referral management. DSM alone does not track referrals to facilitate closing referral loops.
In contrast, electronic referral systems are easy to set up and have shown great success in reducing specialist appointment wait times, as well as reducing the number of inappropriate referrals [7]. With e-referral systems, front office staff waste less time on the phone hunting down important patient referral information. Everyone is informed at every step of the referral process [8] and appointments are accepted and scheduled by specialists over 85% of the time [9].
Cutting-edge practices have already adopted electronic referral systems. Healthcare is using technology to shift towards more efficient processes as new value-based reimbursement systems roll out. Now is the time for your practice to throw your paper referral process away. Reduce faxed referrals to nearly zero, ditch manual communication and go beyond the EHR. The best place to start is with closed-loop electronic referral management.
[1] Archives of Internal Medicine | http://archinte.jamanetwork.com/article.aspx?articleid=1108675
[2] Applied Clinical Informatics | https://aci.schattauer.de/en/contents/archive/manuscript/25997.html
[3] Journal of the American Medical Informatics Association | http://jamia.oxfordjournals.org/content/early/2016/06/28/jamia.ocw067
[4] 2012 IEEE International Conference on Information Reuse and Integration | http://ieeexplore.ieee.org/xpl/articleDetails.jsp?arnumber=6303060&searchWithin%3Dreferral%26filter%3DAND%28p_IS_Number%3A6302564%29
[5] BMC Health Services Research | http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4684927/
[6] New England Journal of Medicine | http://www.nejm.org/doi/full/10.1056/NEJMhpr0706165
[7] “Adopting Accountable Care” | http://www.accountablecarelc.org/sites/default/files/ACO%20Toolkit%20%20Full%20Version%20Text.pdf
[8] ”Reducing Care Fragmentation” | http://www.improvingchroniccare.org/downloads/reducing_care_fragmentation.pdf
[9] Internal Treatspace Metrics